Evaluation of the BNT162b2 COVID-19 vaccine in children 5 to 11 years of age.external icon Walter et al. NEJM (November 9, 2021).
Key findings:
- In children aged 5–11 years, BNT162b2 (Comirnaty, Pfizer/BioNTech) vaccine efficacy for prevention of COVID-19 was 90.7% (95% CI 67.4%-98.3%) (Figure).
- SARS-CoV-2 neutralizing antibody titers 1 month after dose 2 among 5–11-year-olds (10 µg dose) were similar to those among 16–25-year-olds who received 30 µg doses (geometric mean ratio was 1.04, 95% CI 0.93-1.18).
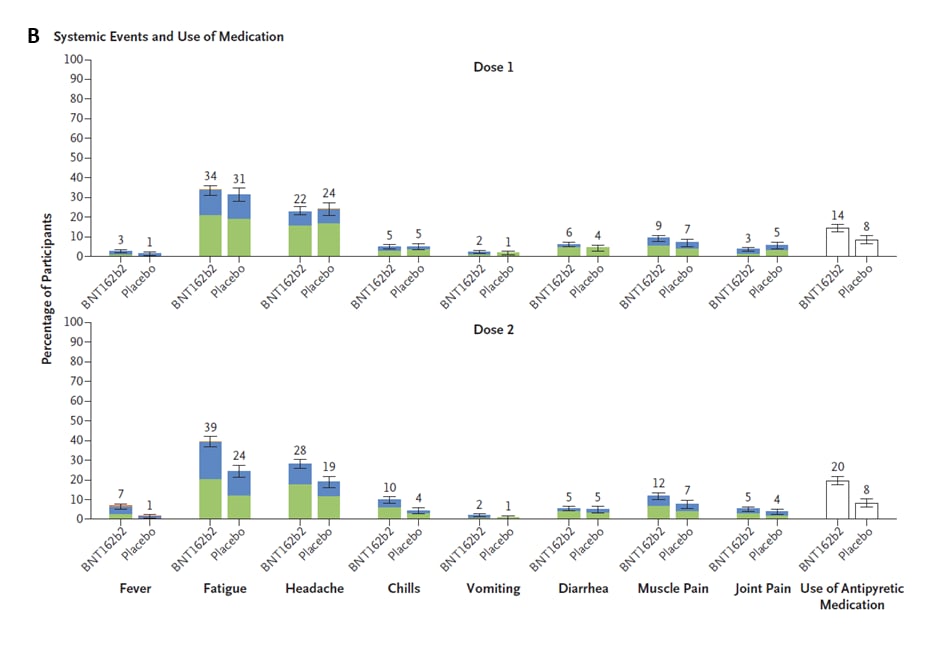
- BNT162b2 10 µg doses had a favorable safety profile among 5–11-year-olds (Figure).
- No serious vaccine-related adverse events were noted.
Methods: Ongoing phase 2–3 safety, immunogenicity, and efficacy trial of BNT162b2 vaccination in healthy children aged 5–11 years. Children were randomly assigned to receive either two 10 µg doses of BNT162b2 21 days apart or placebo; 1,517 received BNT162b2 and 751 received placebo. Vaccine efficacy was assessed ≥7 days after dose 2. Immune responses 1 month after dose 2 were immunologically bridged to those of 16–25-year-old participants from the pivotal trialexternal icon of 2 BNT162b2 30 µg doses. Limitations: Short duration of follow up (median 2.3 months); study likely under-powered to detect rare adverse events.
Implications: Two 10 µg doses of BNT162b2 vaccine were safe, immunogenic, and efficacious in children 5–11 years of age.
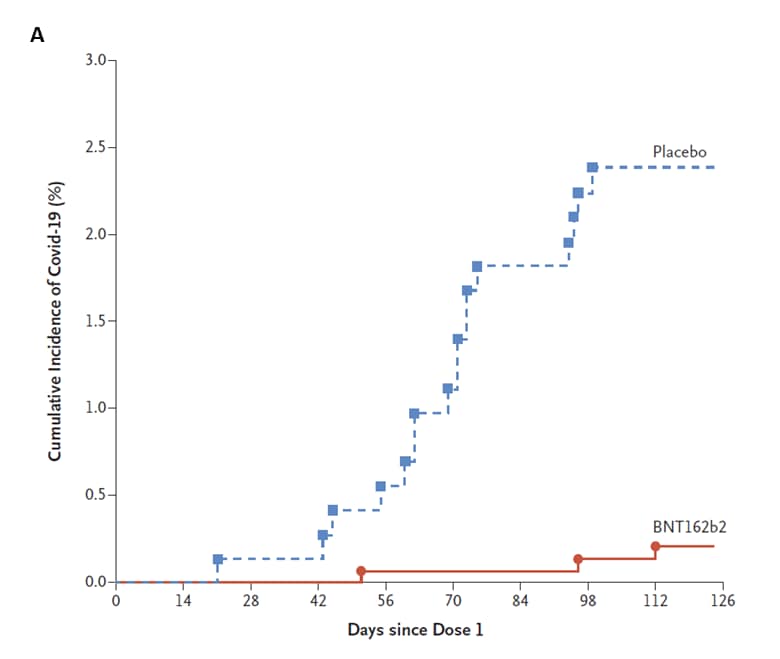
Note: Adapted from Walter et al. Panel A shows the cumulative incidence of the 1st occurrence of COVID-19 after BNT162b2 dose 1 or placebo. Each symbol represents cases of COVID-19 on a given day. Panel B shows systemic events reported within 7 days after vaccine dose 1 (n = 1,511) and dose 2 (n = 1,501) and placebo (dose 1, n = 748 or 749; dose 2, n = 740 or 741 [number of children reporting at least 1 “yes” or “no” for the event after each dose]). Bar colors refer to adverse event severity: mild, moderate, severe, grade 4. Numbers above bars are percentage of participants in each group. I bars represent 95% CIs. From the New England Journal of Medicine, Walter et al., Evaluation of the BNT162b2 COVID-19 vaccine in children 5 to 11 years of age. November 9, 2021, online ahead of print. Copyright © 2021 Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
Distinct SARS-CoV-2 antibody reactivity patterns elicited by natural infection and mRNA vaccinationexternal icon. Assis et al. NPJ Vaccines (November 4, 2021).
Key findings:
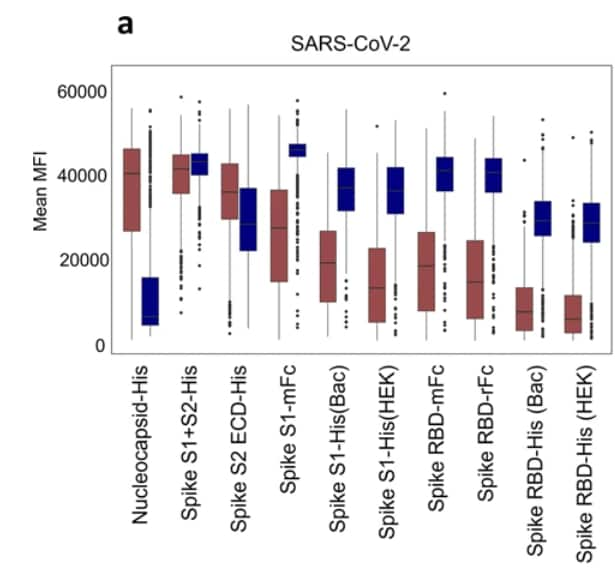
- Specimens from mRNA-vaccinated healthcare workers demonstrated higher antibody levels to the SARS-CoV-2 spike protein S1 and receptor binding domains (RBD) than specimens from a community sample of unvaccinated seropositive persons (Figure).
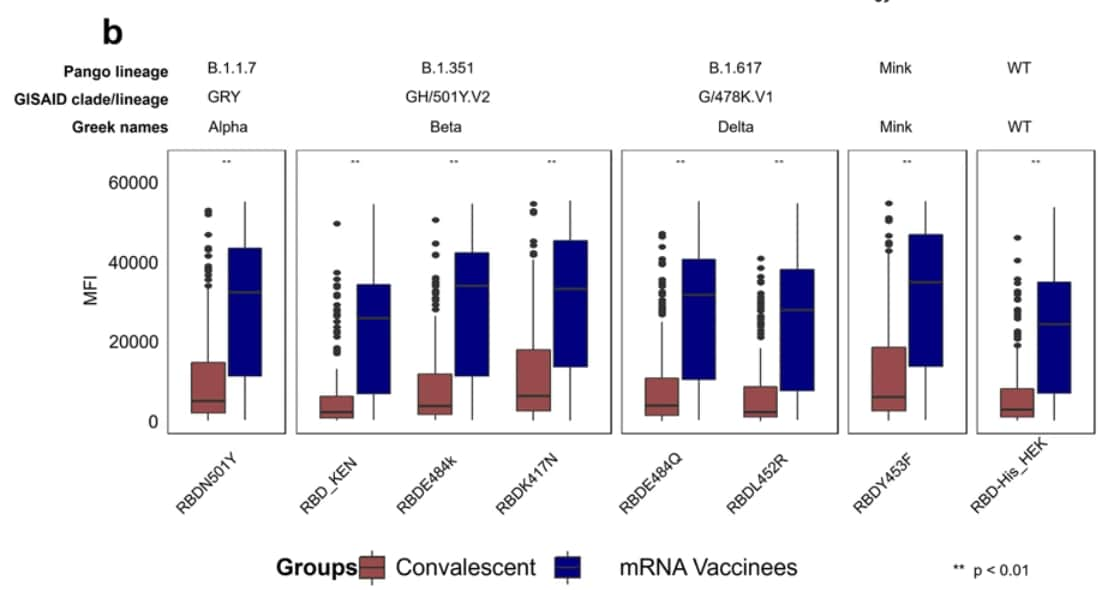
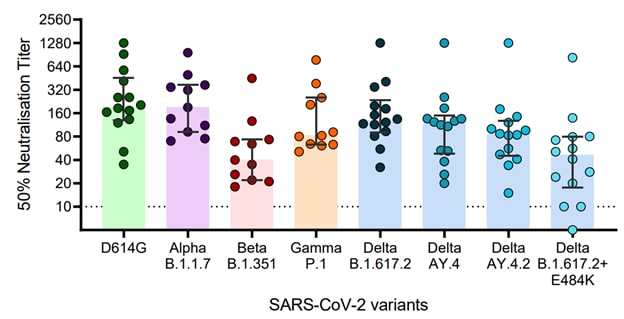
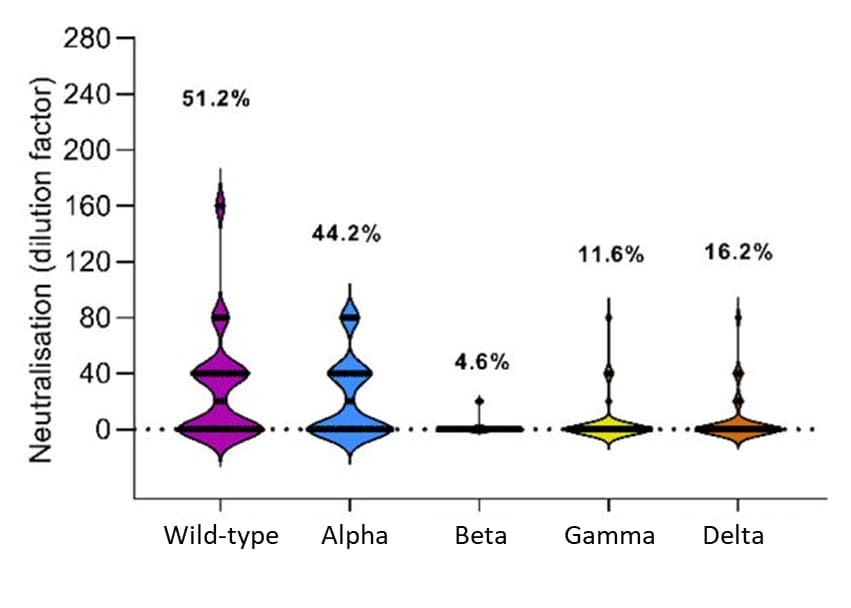
- When exposed to RBD domains from the Alpha (B.1.1.7), Beta (B.1.351), Delta (B.1.617.2), and wild-type lineages, higher anti-RBD antibody titers were observed in plasma from vaccinated persons than in plasma from people who recovered from confirmed COVID-19 (Figure).
- Specimens from mRNA-vaccinated healthcare workers had greater anti-RBD reactivity than specimens from unvaccinated hospitalized COVID-19 patients who required ICU care.
Methods: Samples were obtained from 2 ongoing COVID-19 longitudinal serological surveys of Orange County, CA residents (July and December 2020) and healthcare workers (May and December 2020–March 2021) and a hospital biorepository of samples from 93 hospitalized patients. IgG levels were determined using a multiplex antigen microarray containing antigens from SARS-CoV-2. Limitations: Unclear severity and timing of participants’ infections and timing of vaccination; SARS-CoV-2 exposure may have differed between groups; specimens collected during pre-Delta period.
Implications: mRNA vaccination appears to induce a broader antibody response than SARS-CoV-2 infection.
Figure:
Note: Adapted from Assis et al. Natural exposure (from Santa Ana cohort, December 2020) vs. mRNA vaccination (from February/March 2021 cohort) antibody reactivity against (a) SARS-CoV-2 antigens, and ( RBD from Alpha, Beta, Delta, and Mink variants, and wild-type (WT) virus. Mean fluorescence intensity (MFI) signals for antibodies are plotted. The boxes represent the 1st quartile, median, and 3rd quartile and the whiskers extend 1.5 times the interquartile range (IQR). Wilcoxon test was performed for pairwise comparisons and p values <0.01 were considered significant and represented as **. Licensed under CC BY 4.0.
RBD from Alpha, Beta, Delta, and Mink variants, and wild-type (WT) virus. Mean fluorescence intensity (MFI) signals for antibodies are plotted. The boxes represent the 1st quartile, median, and 3rd quartile and the whiskers extend 1.5 times the interquartile range (IQR). Wilcoxon test was performed for pairwise comparisons and p values <0.01 were considered significant and represented as **. Licensed under CC BY 4.0.
Three doses of COVID-19 mRNA vaccination are safe based on adverse events reported in electronic health records.external icon Niesen et al. medRxiv (November 9, 2021).
Key findings:
- Reports of severe adverse events after a 3rd dose of a COVID-19 mRNA vaccine were rare.
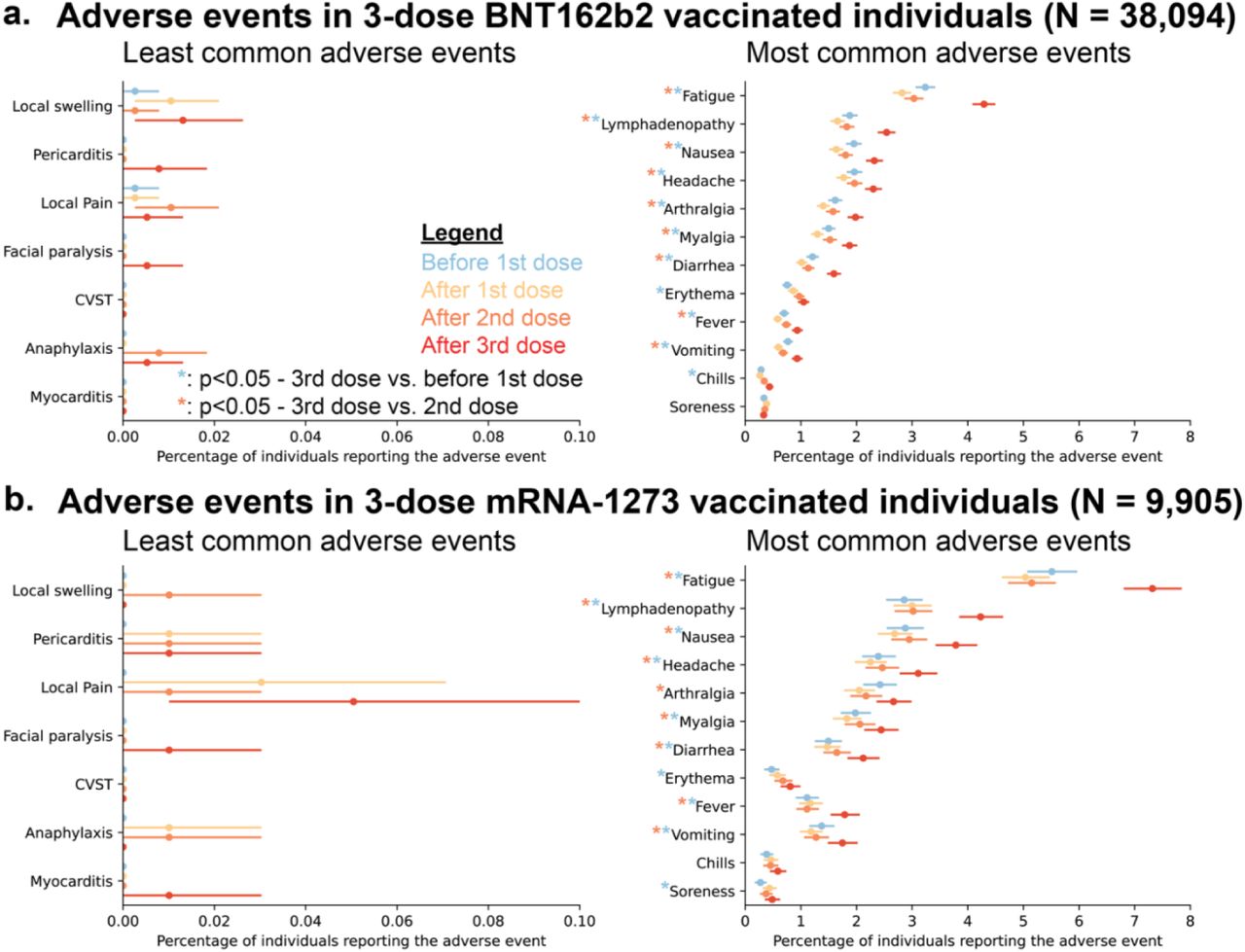
- Pericarditis, anaphylaxis, myocarditis, and cerebral venous sinus thrombosis after dose 3 were reported for ≤0.01% of vaccinated persons (similar to the occurrence after dose 2) (Figure).
- Fatigue, lymphadenopathy, nausea, and headache were reported slightly more often after dose 3 than dose 2 (Figure).
Methods: Retrospective study of patients vaccinated with 3 doses of BNT162b2 (Comirnaty, Pfizer/BioNTech, n = 38,094) or mRNA-1273 (Moderna, n = 9,905), December 1, 2020–October 17, 2021. Electronic health records were used to identify adverse events in the 2 weeks prior to the 1st dose and 2 weeks following the 1st, 2nd, and 3rd doses. Limitations: Limited to signs/symptoms included in electronic health records; persons who experienced post-vaccine adverse events might be less likely to get subsequent doses; results may not be generalizable.
Implications: The risk of severe adverse events after a 3rd dose of COVID-19 mRNA vaccine is low and comparable to the risk after a 2nd dose.
Figure:
Note: Adapted from Niesen et al. Prevalence of vaccine-associated adverse events in 3-dose vaccinated individuals during the 14-day period before 1st dose, after 1st dose, after 2nd dose, and after 3rd dose in (a) individuals that received 3 doses of BNT162b2, and ( individuals that received 3 doses of mRNA-1273. Error bars indicate 95% confidence intervals, and asterisks indicate adverse events with significant (two-tailed p-value <0.05) difference in prevalence after the 3rd dose, compared with before the 1st dose (blue asterisk) or after the 2nd dose (orange asterisk). Used by permission of authors.
individuals that received 3 doses of mRNA-1273. Error bars indicate 95% confidence intervals, and asterisks indicate adverse events with significant (two-tailed p-value <0.05) difference in prevalence after the 3rd dose, compared with before the 1st dose (blue asterisk) or after the 2nd dose (orange asterisk). Used by permission of authors.